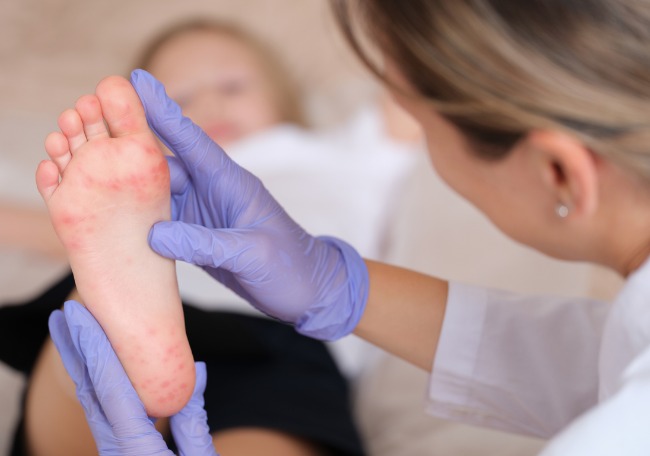
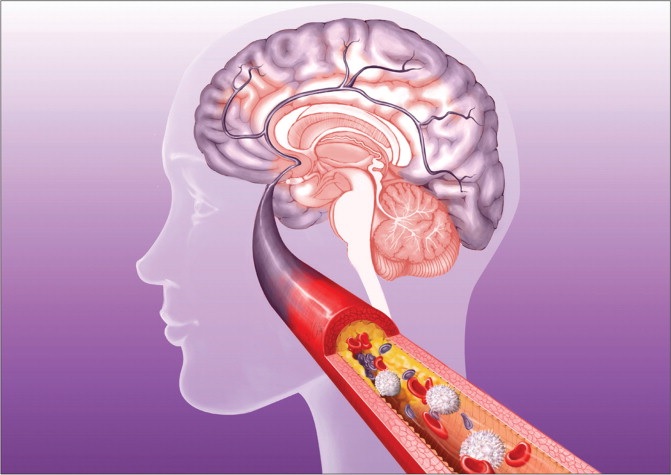
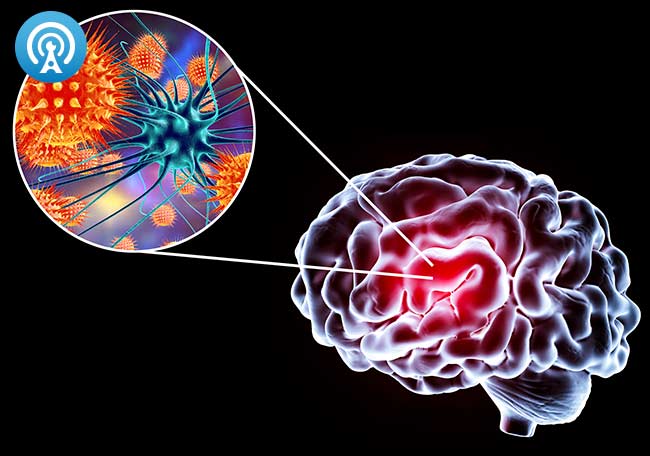
Encefalitis viral aguda
1. Venkatesan A, Tunkel AR, Bloch KC, et al. Case definitions, diagnostic algorithms, and priorities in encephalitis: consensus statement of the International Encephalitis Consortium. Clin Infect Dis 2013; 57: 1114-28.
2. George BP, Schneider EB, Venkatesan A. Encephalitis hospitalization rates and inpatient mortality in the United States, 2000-2010. PLoS One 2014; 9(9): e104169.
3. Vora NM, Holman RC, Mehal JM, Steiner CA, Blanton J, Sejvar J. Burden of encephalitis-associated hospitalizations in the United States, 1998-2010. Neurology 2014; 82: 443-51.
4. Tunkel AR, Glaser CA, Bloch KC, et al. The management of encephalitis: clinical practice guidelines by the Infectious Diseases Society of America. Clin Infect Dis 2008; 47: 303-27.
5. Salimi H, Cain MD, Klein RS. Encephalitic arboviruses: emergence, clinical presentation, and neuropathogenesis. Neurotherapeutics 2016; 13: 514-34.
6. Montgomery RR. Age-related alterations in immune responses to West Nile virus infection. Clin Exp Immunol 2017;187: 26-34.
7. Moraru M, Cisneros E, Gómez-Lozano N, et al. Host genetic factors in susceptibility to herpes simplex type 1 virus infection: contribution of polymorphic genes at the interface of innate and adaptive immunity. J Immunol 2012; 188: 4412-20.
8. Taylor KG, Woods TA, Winkler CW, Carmody AB, Peterson KE. Age-dependent myeloid dendritic cell responses mediate resistance to La Crosse virus-induced neurological disease. J Virol 2014; 88: 11070-9.
9. Long D, Deng X, Singh P, Loeb M, Lauring AS, Seielstad M. Identification of genetic variants associated with susceptibility to West Nile virus neuroinvasive disease. Genes Immun 2016; 17: 298-304.
10. Crosslin DR, Carrell DS, Burt A, et al. Genetic variation in the HLA region is associated with susceptibility to herpes zoster. Genes Immun 2015; 16: 1-7.
11. Qian F, Thakar J, Yuan X, et al. Immune markers associated with host susceptibility to infection with West Nile virus. Viral Immunol 2014; 27: 39-47.
12. Qian F, Goel G, Meng H, et al. Systems immunology reveals markers of susceptibility to West Nile virus infection. Clin Vaccine Immunol 2015; 22: 6-16.
13. Ignatieva EV, Igoshin AV, Yudin NS. A database of human genes and a gene network involved in response to tick-borne encephalitis virus infection. BMC Evol Biol 2017; 17: Suppl 2: 259.
14. Mickiene A, Pakalniene J, Nordgren J, et al. Polymorphisms in chemokine receptor 5 and Toll-like receptor 3 genes are risk factors for clinical tick-borne encephalitis in the Lithuanian population. PLoS One 2014; 9(9): e106798.
15. Lim JK, McDermott DH, Lisco A, et al. CCR5 deficiency is a risk factor for early clinical manifestations of West Nile virus infection but not for viral transmission. J Infect Dis 2010; 201: 178-85.
16. Mørk N, Kofod-Olsen E, Sørensen KB, et al. Mutations in the TLR3 signaling pathway and beyond in adult patients with herpes simplex encephalitis. Genes Immun 2015; 16: 552-66.
17. Verma R, Bharti K. Toll like receptor 3 and viral infections of nervous system. J Neurol Sci 2017; 372: 40-8.
18. Sironi M, Peri AM, Cagliani R, et al. TLR3 mutations in adult patients with herpes simplex virus and varicella-zoster virus encephalitis. J Infect Dis 2017; 215: 1430-4.
19. Lim JK, Lisco A, McDermott DH, et al. Genetic variation in OAS1 is a risk factor for initial infection with West Nile virus in man. PLoS Pathog 2009; 5(2): e1000321.
20. Steiner I, Budka H, Chaudhuri A, et al. Viral meningoencephalitis: a review of diagnostic methods and guidelines for management. Eur J Neurol 2010; 17(8): 999-1009.
21. Solomon T, Michael BD, Smith PE, et al. Management of suspected viral encephalitis in adults — Association of British Neurologists and British Infection Association National Guidelines. J Infect 2012;64: 347-73.
22. Whitley RJ, Soong S-J, Linneman C Jr, Liu C, Pazin G, Alford CA. Herpes simplex encephalitis. JAMA 1982; 247: 317-20.
23. Chow FC, Glaser CA, Sheriff H, et al. Use of clinical and neuroimaging characteristics to distinguish temporal lobe herpes simplex encephalitis from its mimics. Clin Infect Dis 2015; 60: 1377-83.
24. Glaser CA, Honarmand S, Anderson LJ, et al. Beyond viruses: clinical profiles and etiologies associated with encephalitis. Clin Infect Dis 2006; 43: 1565-77.
25. Beattie GC, Glaser CA, Sheriff H, et al. Encephalitis with thalamic and basal ganglia abnormalities: etiologies, neuroimaging, and potential role of respiratory viruses. Clin Infect Dis 2013; 56: 825-32.
26. Xu GJ, Kula T, Xu Q, et al. Comprehensive serological profiling of human populations using a synthetic human virome. Science 2015; 348: aaa0698.
27. Leber AL, Everhart K, Balada-Llasat JM, et al. Multicenter evaluation of BioFire FilmArray meningitis/encephalitis panel for detection of bacteria, viruses and yeast in cerebrospinal fluid specimens. J Clin Microbiol 2016; 54: 2251-61.
28. Simner PJ, Miller S, Carroll KC. Understanding the promises and hurdles of metagenomic next-generation sequencing as a diagnostic tool for infectious diseases. Clin Infect Dis 2018; 66: 778-88.
29. Brown JR, Bharucha T, Breuer J. Encephalitis diagnosis using metagenomics: application of next generation sequencing for undiagnosed cases. J Infect 2018; 76:225-40.
Comentarios
Para ver los comentarios de sus colegas o para expresar su opinión debe ingresar con su cuenta de IntraMed.