|
Resumen
|
Las enfermedades febriles indiferenciadas agudas se caracterizan por fiebre de menos de dos semanas de duración sin síntomas específicos de ningún órgano al inicio. A veces comienzan con cefalea, escalofríos y mialgia.
Más tarde se pueden afectar órganos específicos. Las EFIA abarcan desde una enfermedad leve y autolimitada hasta una enfermedad progresiva potencialmente mortal. La mortalidad es del 12% en pacientes hospitalizados gravemente enfermos en regiones tropicales.
Las EFIA se clasifican en enfermedades palúdicas y no palúdicas con ayuda del microscopio o análisis diagnósticos rápidos para paludismo. La superposición de las características epidemiológicas y clínicas a menudo dificulta el diagnóstico.
El interés se centra más en las EFIA no palúdicas debido a la disminución del paludismo en muchas regiones del mundo. Estas son responsables del 20-50% de todas las fiebres en los niños mayores de cinco años y en los adultos en Asia y África.
La confirmación por los estudios complementarios es difícil, al contrario de lo que ocurre con el paludismo y el dengue. Las recomendaciones actuales no se ocupan integralmente de las infecciones indiferenciadas, lo que puede provocar el empleo indiscriminado de antipalúdicos y antibióticos.
| Causas de las EFIA no palúdicas |
Estudios de Asia y África indican que las infecciones por arbovirus (17,5% de las enfermedades febriles graves), las infecciones bacterianas del torrente circulatorio (principalmente la fiebre entérica) (10,5%), y las zoonosis bacterianas como la leptospirosis y las rickettsiosis (4,0% cada una) son causas importantes de las EFIA no palúdicas.
La fiebre entérica afecta a 11,9 millones de personas por año en Asia y África. Más de un millón de casos de leptospirosis y otro tanto de tifus de los matorrales se producen anualmente en todo el mundo
El siguiente cuadro muestra las EFIA frecuentes y sus causas.
Cuadro1: Los cinco grupos principales que causan enfermedades febriles indiferenciadas agudas
|
Paludismo—Incluye el paludismo debido a Plasmodium falciparum, P vivax, Povale, P malariae, P knowlesi. |
Son infecciones más raras las fiebres hemorrágicas virales, como la enfermedad por el virus del Ébola, la fiebre de Lassa en África y la fiebre hemorrágica de Crimea-Congo (FHCC) con distribución más amplia.
Recientemente se comprobaron brotes de esta última, también llamada virus asiático del Ébola en Pakistán e India con alta mortalidad. El reconocimiento precoz de estas enfermedades es importante, ya que causan alta mortalidad y se diseminan rápidamente.
| Diagnóstico |
Es conveniente seguir una estrategia escalonada para sintetizar la información sobre los antecedentes y la epidemiología. La anamnesis y el examen físico cuidadoso pueden proporcionar claves esenciales. Los médicos en zonas con acceso limitado a pruebas diagnósticas tendrán que confiar solo en estos para formular un diagnóstico probable y comenzar el tratamiento. Véase la figura

En el paso 1 se debe considerar el factor estacional porque algunas infecciones son más frecuentes durante la estación de las lluvias.
Dentro de las zonas que se consideran endémicas, la epidemiología de las EFIA continúa evolucionando. El tifus de los matorrales y la leptospirosis, que antes se consideraban enfermedades rurales, ahora afectan también a las poblaciones urbanas.
Los parques urbanos y las inundaciones en villas y barrios pobres han surgido como factores de riesgo para estas enfermedades.
El dengue, antes considerado una enfermedad urbana, se observa cada vez más en zonas rurales y periurbanas en India. La melioidosis es una causa importante de sepsis extrahospitalaria en el norte de Tailandia y de Australia, y actualmente es endémica en muchos países del subcontinente indio, Asia del este y África subsahariana.
| Posibles exposiciones |
Es necesario interrogar sobre:
• Picaduras de insectos o mosquitos, responsables de la transmisión de varias infecciones (paludismo, dengue, chikungunya, Zika, FHCC, tifus de los matorrales, tifus murino, rickettsiosis exantemática, fiebre recurrente).
• Consumo de alimentos y agua contaminada, responsables de la fiebre intestinal. .
• Contacto con líquidos corporales o productos de animales o agua y tierra contaminadas, a través de excoriaciones de la piel o las conjuntivas, vinculados con la leptospirosis.
• Caminar descalzo, trabajar en arrozales, inundaciones en zonas urbanas, que son factores de riesgo del tifus de los matorrales y la leptospirosis. En las zonas rurales pueden coexistir los riesgos de exposición a múltiples vectores.
| Inicio, duración y características de la fiebre y la enfermedad |
El dengue tiene un curso autolimitado con fiebre que dura hasta 7-12 días
Las características de la fiebre pueden cambiar debido a la acción de medicamentos antifebriles como paracetamol e ibuprofeno, pero a veces pueden ser típicas de una infección específica.
• El paludismo, las infecciones por arbovirus, el tifus de los matorrales y la leptospirosis tienen un comienzo abrupto y pueden progresar rápidamente a complicaciones en la primera semana. En el paludismo debido a Plasmodium vivax or P ovale se observa día por medio un pico en la temperatura
• La fiebre intestinal es de comienzo más insidioso. La fiebre >39°C durante más de tres días con dolor abdominal y diarrea o constipación sugiere fiebre intestinal.
• El dengue tiene un curso autolimitado con fiebre que dura hasta 7-12 días.
• La fiebre de la gripe clásicamente dura tres días, pero puede persistir hasta ocho días.
• La fiebre puede estar ausente o ser solo febrícula en la infección por Zika.
• Las borreliosis tropicales causan fiebre recurrente que dura 3-5 días entre períodos afebriles de 4-10 días.
| Factores relacionados con el paciente |
La edad, las enfermedades concomitantes, la inmunosupresión y el embarazo pueden contribuir a estrechar el diagnóstico diferencial y también afectar la evolución.
Por ejemplo, los pacientes con diabetes tienen mayor riesgo de melioidosis. La bacteriemia debida a la Salmonella no tifoidea, la tuberculosis diseminada y las micosis profundas se observan con mayor frecuencia en adultos con infección por VIH.
La inmunosupresión relacionada con el embarazo genera mayor gravedad de las infecciones, en especial con el paludismo por P. falciparum.
Examen físico
Evaluar la gravedad de la enfermedad
Se deben buscar signos de enfermedad grave (cuadro 2) que indican la necesidad de hospitalización urgente.
Cuadro 2: Signos de alarma en pacientes con enfermedades febriles indiferenciadas agudas que indican la necesidad de hospitalización y tratamiento urgentes
|
• Postración—Incapaz de pararse, sentarse o caminar sin apoyo |
> Descartar las infecciones circunscritas
Evaluar a los pacientes con fiebre, infección especialmente grave, tanto para infecciones circunscritas como para EFIA. La gripe se puede confundir con las EFIA ya que la fiebre y la mialgia pueden desviar la atención de los síntomas respiratorios, que quizás estén ausentes en los adultos mayores. Las complicaciones de las EFIA también pueden imitar a las infecciones circunscritas—como el paludismo por P. falciparum (encefalitis), el tifus de los matorrales (neumonía grave), o la leptospirosis con ictericia (infecciones hepatobiliares).
> Buscar indicios diagnósticos de las EFIA
Ciertos signos en el examen físico ayudan a limitar los diagnósticos diferenciales. Estos signos, de estar presentes solos o en combinación con otros, indican una probabilidad de moderada a alta de una EFIA en especial.
El tifus de los matorrales produce una lesión cutánea característica—una escara — que se observa en el 17-57% de los pacientes según informes de India y en el 56-86% de los pacientes en informes de otras regiones asiáticas. Examine cuello, tórax, axilas, abdomen e ingles en busca de estas lesiones que no son dolorosas ni pruriginosas.
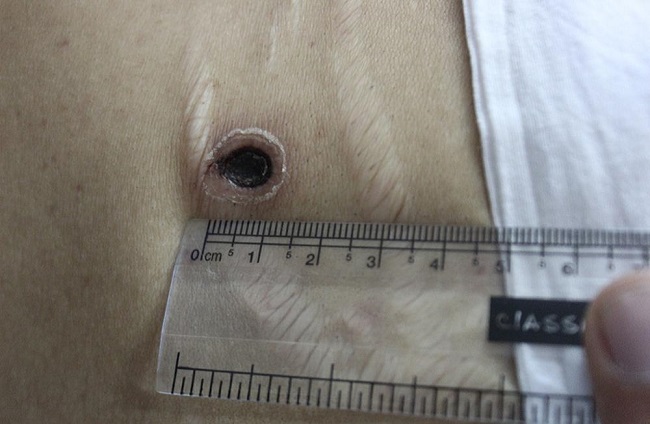
Fig 2 Escara abdominal. Obsérvese la úlcera en sacabocados característica con una escara negra en el centro
Una lesión similar en un paciente con enfermedad más leve en África sugiere la fiebre africana por picadura de garrapata, observada con frecuencia en viajeros que vuelven de las reservas de caza. La falta de dolor y edema en las escaras debidas a la infección por rickettsias las distinguen de aquella de causas más raras, como tularemia, ántrax, o tripanosomiasis del África oriental.
La sufusión conjuntival (ojos rojos y edema sin exudado) y la hemorragia, ictericia y fuerte dolor con la palpación muscular sugieren leptospirosis. También se observa conjuntivitis no purulenta con frecuencia en la infección por el virus Zika. .
El exantema y/o la poliartritis sugieren infecciones arbovirales como dengue, Zika o chikungunya. En la infección por virus Zika, aparece un exantema maculopapular en el primer día, con distribución cefalocaudal y acompañado de prurito intenso, que empeora al dormir.
En cambio, el exantema del dengue aparece primero en el tronco alrededor de cinco días después del inicio de la fiebre. La artritis simétrica de las pequeñas articulaciones con edema es típica de la chikungunya.
A la inversa, ciertos signos excluyen una enfermedad en especial. Por ejemplo, un exantema o adenopatías es muy improbable en el paludismo. Asimismo, las adenopatías son infrecuentes en la fiebre intestinal. La ictericia con fiebre alta hace menos probable el diagnóstico de hepatitis viral y en cambio sugiere leptospirosis u otras EFIA con compromiso hepático.
| Los primeros exámenes |
En zonas endémicas se debe pedir un hemograma completo, análisis de orina, y microscopía del frotis y/o una prueba diagnóstica rápida para paludismo en todos los pacientes con fiebre. El examen de orina puede revelar infección urinaria, a veces asintomática en mujeres y ancianos.
Las pruebas de función hepática y renal y los estudios por imágenes (radiografía y ecografía) son útiles en pacientes con síntomas delimitados y en pacientes graves, para detectar complicaciones. Según el diagnóstico presunto se pedirán análisis confirmatorios para infecciones específicas.
Las infecciones por espiroquetas y rickettsias se confirman por la demostración de una seroconversión de la IgM (aparición de IgM en muestras tomadas alrededor de 10 días después de la muestra anterior), o la cuadriplicación del valor de IgG en un par de muestras con por lo menos dos semanas de intervalo entre ellas.
Esto impide su empleo en la toma de decisiones inmediata. Estas pruebas tienen limitaciones en la disponibilidad y la sensibilidad. Por ejemplo, la sensibilidad del hemocultivo y la PCR son más altas en la primera semana. La especificidad de las pruebas serológicas se afecta por las reacciones cruzadas entre los agentes patógenos y por la persistencia de anticuerpos IgM tras las infecciones.
En la práctica entonces no hay certeza diagnóstica ante una EFIA no palúdica. La demostración de anticuerpos IgM en una sola muestra en la fase aguda contribuye cuando mucho a un “diagnóstico probable” de leptospirosis y tifus de los matorrales.
| Complicaciones |
El paludismo, el tifus de los matorrales y la leptospirosis pueden progresar rápidamente a la disfunción multiorgánica dentro de la primera semana. El tifus de los matorrales y la leptospirosis graves se pueden manifestar como neumonía bilateral o hemorragia pulmonar respectivamente y evolucionar al síndrome de dificultad respiratoria aguda.
El tifus de los matorrales es una causa importante de fiebre en mujeres embarazadas en Asia y se asocia con altas tasas de abortos espontáneos (17%) y mala evolución del recién nacido (42%).
El dengue habitualmente se resuelve en una semana. Las complicaciones como shock o hemorragia se producen 3-5 días después del inicio de la fiebre.
La fiebre intestinal tiene inicio subagudo con complicaciones como encefalopatía, perforación intestinal y hemorragia solo en la segunda o tercera semana de la enfermedad.
Sin tratamiento, el índice de letalidad es del 2,49% en la fiebre intestinal, del
0 al 39,7% en la leptospirosis ictérica y del 0 al 33% en el tifus de los matorrales.
| Tratamiento |
> Pacientes estables
Los pacientes estables sin señales de alarma no necesitan hospitalización. Aquellos con diagnóstico confirmado de malaria o dengue se tratarán según las guías nacionales.
Para las EFIA con características clínicas presuntamente bacterianas es prudente iniciar tratamiento precoz con antibióticos mientras se aguardan los exámenes complementarios o estos no están disponibles. Infecciones como las rickettsiosis y la leptospirosis progresan rápidamente y la demora en el tratamiento puede aumentar su gravedad y mortalidad.
En zonas que son coendémicas para rickettsiosis y leptospirosis, especialmente en el sudeste asiático, la doxiciclina es una opción apropiada. La azitromicina oral es eficaz para la fiebre intestinal sin complicaciones, el tifus de los matorrales, la leptospirosis y la fiebre recurrente. La doxiciclina oral no se aconseja durante el embarazo.
> Pacientes graves
Estos pacientes se deben hospitalizar inmediatamente. El tratamiento empírico con una cefalosporina de tercera generación (ceftriaxona) por vía parenteral junto con doxiciclina o azitromicina es apropiado mientras se aguarda la confirmación diagnóstica.
La ceftriaxona es para la fiebre intestinal y la leptospirosis; la doxiciclina para las rickettsiosis. Esta combinación también es apropiada para las EFIA complicadas por neumonía o por el síndrome de dificultad respiratoria aguda, la encefalopatía y la afectación hepática y no es necesario modificar la dosis en la insuficiencia renal y la insuficiencia multiorgánica.
También se la puede administrar en pacientes ante la sospecha o el diagnóstico de paludismo grave, además del artesunato intravenoso.
Es importante conocer las características locales de la resistencia. Por ejemplo, se documentó fiebre tifoidea resistente a varios ATB en Pakistán desde 2016, por lo que se deben emplear carbapenems o azitromicina. Además, las características locales de las enfermedades orientan las opciones terapéuticas.
Por ejemplo, en pacientes con EFIA seguida por una neumonía grave, si hay una epidemia de gripe sería prudente agregar oseltamivir hasta que se confirme la gripe con pruebas de antígenos o prueba rápida de PCR. En zonas donde la melioidosis es común, ceftazidima o meropenem pueden ser una opción inicial apropiada.
> Continuación del tratamiento
La respuesta de la fiebre a los antibióticos varía: las infecciones por Rickettsias suelen responder dentro de las 48 horas, mientras que puede tardar hasta una semana en la fiebre intestinal y más aún en la melioidosis
. Los resultados del hemocultivo o de las pruebas serológicas confirmarán el diagnóstico y orientar el tratamiento.
Aunque la fiebre responda al tratamiento empírico, una nueva muestra varias semanas después demostrará la seroconversión de la IgM o la cuadriplicación de los valores para confirmar el diagnóstico. Este se debe reconsiderar si la fiebre persiste tras la antibioticoterapia apropiada.
Resumen y comentario objetivo: Ricardo Ferreira